For a rare occasion, I can honestly say I had my stuff together by the evening of Sunday, March 6th. Earlier that day, our family had attended our first St Baldrick's event, hosted by St. Joseph's Church in Camillus. I spoke at the event, we connected with other local cancer families and little William got his picture taken with six other warriors!
After a whirlwind weekend, I was excited for Monday and had all my stuff in order. All laundry was caught up and back in its home in closets and drawers, the house was tidied up, Nicholas' backpack was ready at the door...I even had clothes laid out for the boys and I. We had a fun-filled Monday planned and many other highlights for the week to come.
William had a difficult Sunday night, so I ended up sleeping with him. When I heard the plow come down our street around 5am, I wondered how much snow we had gotten. I never would have expected a snow day in March....but yes, it happened.
Just with the unexpected weather, our day dramatically changed. The housekeeper cancelled, Aunt Elaine was unable to make it for our planned afternoon funnel cake party, I cancelled plans with Jodi to see her newborn baby I've been dying to see (and to bring my god-daughter's very overdue Christmas presents)....and we haphazardly figured out a plan to get the boys and I through the day.
In the afternoon, we played outside in all the newly-fallen 18 inches of snow. Nicholas has been begging to make a snowman, but this snow was not the packing-type. We compromised by making a "Lego-snowman" using the snow brick maker.
Nicholas was really proud of our creation - and creatively named Lego-man "Nicholas."
Truthfully, William is not a huge snow fan. He basically went outside with us because he wouldn't have liked the alternative (to be separated from Mommy)...so needless to say, he obliged. He was rather intrigued with the snowman's sweet potato nose and kept trying to go after it (as Nicholas was screeching, "No William, you are going to knock-down my Lego Nicholas man!")


That evening, we all went to Wegman's to grab dinner and do a much-needed grocery shopping. By 6pm, William was at the end of his rope. After eating a nice smorgasbord of rice, green beans, turkey from Mommy's sandwich and sharing a leprechaun cookie with Mommy and Nicholas, William cried until he was carried through the entire remainder of the shopping trip. He was attached to a second hydration pump for the day because I feared he looked slightly dehydrated (he had terrible diarrhea all day...like 9 times in a day).
William woke three times between 8:30pm and 11pm. At 11, he felt warm and was acting a little odd. His temperature proved to be elevated - at 100.5. For most 21-month olds, that temp is nothing concerning, could even be from teething. Knowing William was due for his weekly lab draw at 8:30am Tuesday (literally, 9 hours away), I figured I could give him a dose of Motrin to get us through the night. Lord knows, heading to the ED in the middle of the night is anything but fun.
I stayed with William after giving him the Motrin. Because he is a cool cucumber and consistently runs right around 96.5 degrees, by 101 he was really stressing with increased respirations and a very rapid heartbeat. He did not sleep, but rather laid there about a foot away from me in bed, just staring at the side of my pillow. He did not seek out putting his hand down my shirt...I
knew something was brewing.
Repeatedly I took his temperature, each time he cried "owie, owie" with just having an axillary temp done.
My stress was instantly confirmed as soon as the thermometer started its high alert chime. My heart sank to my stomach when it then glowed 103.1 at 12:45am.
As instructed to do, I paged Dr. Rivera (who did not return my call) and then spoke with Dr. Wali, the GI doctor on call. He instructed me to go to the ED and to expect to be admitted due to the excessive temperature.
Fred and I instantly go into packing mode. He packed the items he knows I always need and then held William following me through the house as I had to pull together additional items. Poppie came over to our house and decided to go to the ED with William and I.
On the ride there, William stayed awake the entire time. His eyes big and wide alert. The ED staff rushed us in, promptly took William's vitals...and would you believe - no temp. I looked at my dad and said, "God, why are we here....should we just leave now?"
At 3am, I literally considered walking out of the ED.....even envisioned myself picking up William and going. Being there with him is virtually signing him up for a whole lot of trauma....bloodwork and cultures off his central line, a peripheral needle stick to run cultures, a urine catch (depending on the attending ED doc, it could mean a sterile urine catheterization or a bag collection), a chest x-ray....and of course repeated blood glucose sticks because William's glucose is certain to drop during or after a high fever.
The only thing that stopped me from leaving was recalling how odd William had been staring at home. Even his staring in the truck was just not expected for a boy who had hardly slept a wink all night.
And so the process began: history with the triage nurse and the nurse assigned to William, an interview and exam with the ED med students and residents...then all of the above repeated with the ED attending...cultures, 2 attempts at a peripheral draw, a chest x-ray, urine bag collection....and of course, the tried and true drama of a concerningly low glucose level of 38 while TPN was running. Admittedly, the staff this time around worked well and promptly. William had his two antibiotic runs started within 2 1/2 hours of us getting there.
Randomly, William was comforted best with this snack bag of Goldfish crackers I grabbed as we left the house. He would not let go of that bag - he clutched it with all his little might and nibbled on a half dozen or so crackers through the peripheral ordeal.

Experience has taught us if they can get an IV in while doing the blood draw, we go for it. William's single lumen central line has proven to be more of a problem than a benefit....especially now that his TPN runs 16 hours a day.

After being in the ED for 7 hours, we were admitted in-patient for "observation." The insurance receptionist explained that an observation admission means we may only be there for a few hours or less than a day, but the doctors want to keep an eye on William. I thought this was interesting, since we've never been admitted under this title....but whatever.
At 10am, we were just getting upstairs to our home-away-from-home in Peds Unit 11E. All our familiar faces greeted us and I was relieved to find out Gail was William's assigned day nurse. She is definitely one of the best nurses of the unit and knows us well.
William was pretty tired once we got settled and drifted off to sleep in between all the nurse, med students and resident exams. The head resident even told me he had already talked to Dr. Rivera and they were not planning to continue additional antibiotics until we had growth in his cultures (mind you, this can take days for growth). I really started to question if we needed to be there.
Around 12:30pm, William started an odd moaning. He got very fidgety, couldn't seem to get comfortable, repeatedly said "owie, owie" and I could feel him starting to shiver. His chills became more evident, sometimes with his teeth even chattering and his hands and feet quickly became modeled. Our nurse got right on things....immediately slapping leads on William & hooking him up to the monitor, she took his temperature (which suddenly was 104 degrees), checked his capillary refills (which were poor) and had another nurse page the resident to our room ASAP.
By this point, William's heart rate was consistently in the 190's or above and his respirations between 50-60 breaths a minute. The head resident, Dr. Mittigia, seemed concerned with William's presentation. He had the SWAT team from the PICU paged, ordered a bolus of fluids and continuously checked William's cap refills. He went up to the PICU to talk to the attending and said he would be back in 3 minutes.
Within those 3 minutes, William took a major turn for the worse. His chills got much more dramatic and he had a few episodes that he seemed to be getting shocked from an internal source. He'd suddenly have a major chill come over him, his arms and legs with stiffen up and throw out into extension, his whole body shook, he's do a loud scared moan, gasp his breath... and then grab his chest saying owie as the episode was ceasing. Saying this was incredibly scary would be an understatement....and even with a room full of medical staff present there, nobody seemed to know what to do. These episodes just kept coming, increasing in intensity.
Around this time, the PICU nurse came running in and Dr. Mittigia took charge and said he was pretty certain William was having febrile seizures.
During our conversation, the next seizure was a doozie. It seemed like William couldn't breathe. He was shaking, his body stiff, eyes rolled back in his head, the monitor was going crazy with alarms screaming and I just nearly lost it. I was staring at the monitor and honestly could not even read it. It was like the numbers and lines were jumping all around. The staff told me to put William on the bed. They shoved the crash cart into the room and started William on oxygen....and still I could not read the monitor - these same monitors I've been dealing with for the past 15 months.
I literally began seeing my own life flashing before me. Ya know how you hear the stories from people in near-death experiences.....well, I'm telling you, I saw my own life flash. I yelled, "DO SOMETHING! What is happening.....this is not how this is supposed to happen! What is going on!!!"
My dad was there, once again, by my side through another huge trauma. I couldn't even look at him....he was hardly holding himself together, but tapped my back saying, "He's breathing....he's okay."
I really think if it were anyone else telling me that, I wouldn't be able to believe them....thank god my dad could at least read that damn monitor.
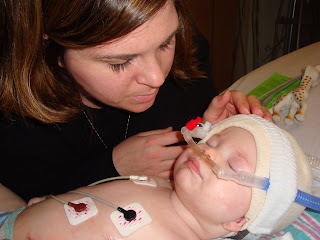
The PICU attending, Dr. Ragosta, came and ordered a glucose bolus and another fluid bolus. William's vital signs were not improving and his capillary refill was still 4-5 seconds. William looked so pale he had a grayish hue. He looked lifeless laying there on that bed. We had nearly the entire staff of the floor outside our door looking in....literally everyone there knows and loves our William.
Eleven hours after his blood cultures in the ED, William's peripheral culture came back growing a gram negative bacteria. Gram negatives are very dangerous blood infections - finding it circulating in his bloodstream confirmed William had septicemia. He had gone into septic shock and experienced febrile seizures.
~
A year an a half ago, I could have written an entry just on how an unexpected snowstorm in March turned our day up-side-down. In our world now, major things can happen in what seems like a heartbeat. During the day, William played nicely, was outside in the cold for well over an hour, was dragged to the grocery store and pretty much had what could be a typical day for any 21-month old. A random fever that quickly spiked and an overly in-tune mother who worried about odd staring brought us to the ED. Within hours, my baby laid on a hospital
bed with his heart racing at 220 beats per minute, seizing and in critical septic condition.
We remained in-patient for 8 days with this infection. William grew two dangerous gram negative blood infections: Klebsiella pneumoniae and escherichia coli. After a consultation with the director of Infectious Disease, they are approximating a 10 percent chance we will be able to fully clear this infection and salvage William's central line. Due to his expected long-term need for a central line and the fact that this is already his third line, William's team collectively agreed to attempt to clear the line with two weeks of IV antibiotics. There are a limited number of veins in one's body for central line access....we must give this our best effort in order to maintain access for William's long-term needs.
The decisions we are constantly finding ourselves in and the needs for continuous advocacy for William's well being is incredibly challenging....and heartbreaking all at the same time. It's hard to even think about the reality of living in this world of great medical frailty. I often feel like I'm on a tightrope of paranoia while attempting to carry what feels like the weight of the world on my shoulders.